A few weeks ago I joined some groups such as “genyus”, whom of which have greatly helped my adjustment after the stroke and coping daily with others who understood. Inspired by groups like them, I wanted to talk about some of the challenges young stroke survivors that people born between the early 1980s to the early 00s might relate to.
We’re not kids but we also probably haven’t had some major life experiences as our more mature young stroke survivors (giving birth…yet etc). We also love technology! Oh, and we are super energetic (well, we try to be lol) Ok, this is being super stereotypical but seriously wanted to talk about others like me even though all of us are certainly different we are also alike.
This is written for 25 to 30 something-year-olds but if you’re a bit older and can relate I would love it if these tips helped you too 🙂 Here are some things I’ve learned from my own experience:
Sleep
Most young stroke survivors find it hard to sleep. Even though we fatigued easily during the day and feel tired…weird huh? I love this Calm app that I found Android and found that it really helps. I listen to “meditative sleep stories”..
Exercise
Again, something I use on my android phone (you can even go a step further and get a fit bit something like that). I use google fit, it automatically counts my steps throughout the day and I add my exercises. I currently do 4km in 12 minutes on the cross trainer (starting the intensity at level 1 for the first 3 minutes, then level 2 at 3 to 6 minutes, level 3 at 6-9minutes and finally, at level 4 9 to 12minutes); 10 minutes on the treadmill (about 800m) and 5-6 minutes on the rowing machine (or equivalent to at least 500m).
I set the goal of at least 30 minutes of exercise every day if I can. Then I add a few minutes every day doing some balance exercises on a balance mat. I guess the theme for me surrounds complacency – do not get complacent!
Diet
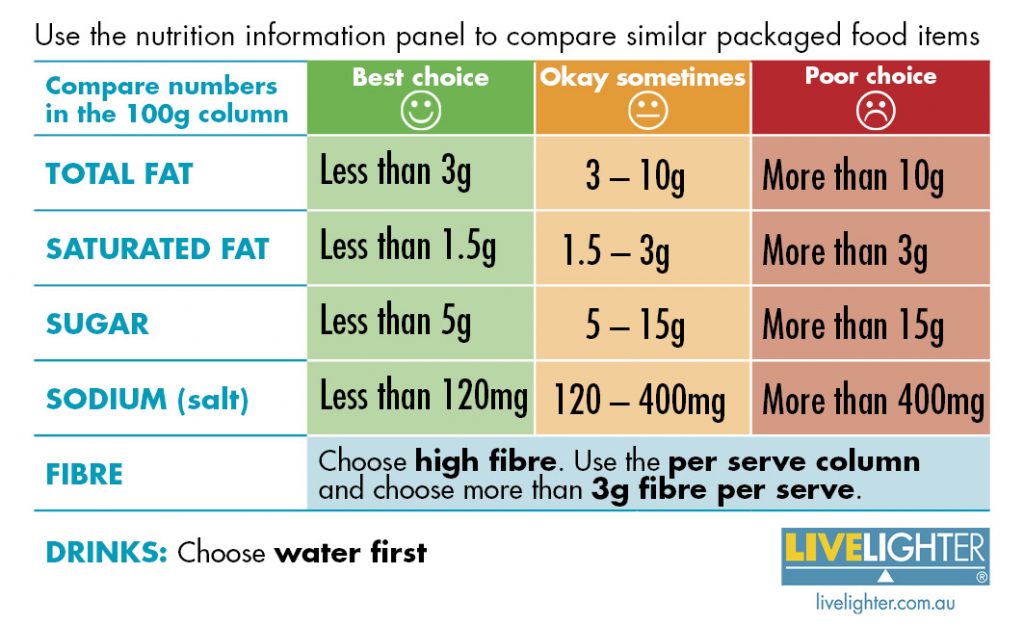
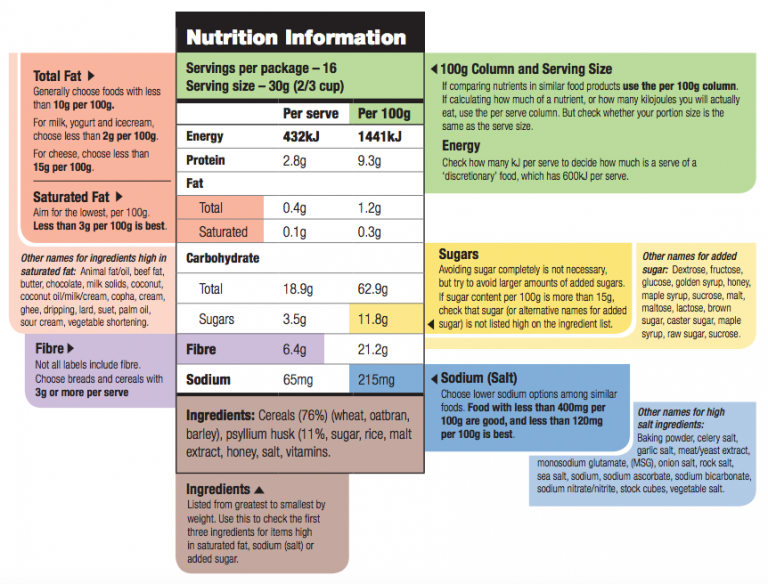
Before the stroke I had relatively healthy habits, even bordering on vegan, but since the stroke and being put on warfarin I cannot any green, leafy vegetable or anything high in vitamin K. As usual diet restrictions note, everything in moderation but definitely NO soft drinks, alcohol or overly processed foods (bye maccas/McDonalds!).
Mental workout
Every day I do a day of challenges set by the android app Elevate and read a lot, here are some great, inspiring books (I haven’t read all of them…yet).
Pregnancy
Like many young women at our age, also known as birthing age, pregnancy is a big question on my mind and while I don’t have all the answers and probably no one does know everything, joining a group really helps to alleviate fears and ask questions. Try joining groups like I did for example: Folks with strokes (Mothers).
Work
Getting back to work is certainly a challenge, not just mentally but physically too. Having a supportive team, boss and partner can definitely help the transition. I have been back now for about month. I have noticed that although I am much slower, I can do it. The physios and psychologists recommended me to go back but with limited expectations.
Where I could write 4 blogs a morning for other companies, I can now only write one in the morning as I find it hard to focus after and I get fatigued/tired easier. So I only work half days at the moment. They also suggested that every hour I take a few minutes to rest and do something else, like walk around, do some squats, stretches and re-focus my eyes (being a copywriter my eyes are always on a screen).
I have an international license but they drive on the other side of the road in the Philippines than in Australia. So you can imagine that is confusing even without having a stroke. I don’t have any tips around this but I have been told after a stroke you are not to drive for several weeks after.
Getting Around
- Just like with my autoimmune condition, I always think of the “Spoon theory”. You have limited spoons now, no more unlimited spoons like before, so pick and choose your battles or outings.
- Heading out tonight? It might mean skipping that afternoon run. If you’re planning to go to a party tomorrow night, make sure you rest up before then to conserve energy.
- Use your phone reminders – I always seem to forget to take medicine on time, so make sure you have a regular alarm to remind you.
- Remember safety first and go slowly! If you are on warfarin too, avoid accidents like cutting yourself or falling down. The first few weeks getting out of rehab, my hubby helped me to walk everywhere (he was the ultimate spotter) but when I am by myself, I am extra careful and cautious of where I am. No rushing! That train or bus can wait or you can catch the next one, do not risk falling over! Not only do you now bleed easier but you also have uncoordinated movements that unexpected falls could make you severely dizzy or worse, cause another stroke! Heaven forbid!
Music
I absolutely love music and it certainly helps in the path towards recovery. Check out my Spotify playlist and you can add your own tunes too >
Challenges
Each month I set a goal to work towards. Next month I am joining a 5km fun “run” (or walk in my case).
Diary
Instead of comparing to what you looked/acted like before the stroke, compare yourself just after the stroke. I could hardly walk or talk, so when I look at it this way, I’ve come a long way!
Sure, if I compare to before there is a big difference, I am a lot slower and unsteady now but I am slowly improving every day, even if it is the subtlest of changes.
Also keeping a diary is super therapeutic, you need to face your feelings not hide from them. Observe them! If you’re angry, why? Go through the motions and express them in your diary, this can be a good log for looking back and also you can see if your handwriting improved too (mine was terrible just after the stroke, well still is haha).
Remember “the more you do, the more you are”. So, don’t let yourself forget how to write, you need to write! It might look super messy in the beginning but after constant practice, it gets better. Even if you didn’t have a stroke, if you didn’t write for a long time, you would find it hard to write neatly again.
Finding your voice
Just after my stroke I lost my voice, literally, at first it was really hard to make sounds, then the words were mixed up, and then I just ended up really husky and breathy like I just had a cough or something.
Before the stroke, I loved to sing so you can imagine losing my voice was definitely a challenge! With a series of vocal exercises (such as a bottle filled with a little water and straw) I have slowly built my voice back and this coming Monday I will see an ENT to do a vocal clinic test to see how the stroke impacted on my vocal chords. I have done previously, but it was not to the extent of my ability to sing.
Currently, I can hum a tune, which is a huge deal! But I can’t hit higher notes or access my mid-range which I see as a part of my voice is paralyzed, or frozen, it feels tighter than usual. I have come across a couple of sites in the meantime: Dysarthria and Singing.
Why not me?
The doctors believe thrombosis caused by my autoimmune disease caused the stroke. But why? I thought to myself. It’s rare I found out. In a video I once posted on my personal social media, I told the story of one night at like 3am I looked in the mirror and I was angry. I kept asking “why me?” but the question I then changed it to was “why not me?”. It is a powerful thing to look in the mirror and ask why not, instead of placing blame on someone else or something else, it’s on me, which leads me to the “real” why question, the “why” that I could control. “Why did you survive?” and it’s up to us to answer that, we are survivors for a reason, hold onto that and keep going!
Emotional Rollercoaster
It may seem that I am not that bad, well let me just start by saying thank you, I work hard at appearing “normal”. Sure I have my days, ups and downs, challenges just like any other stroke survivor, what keeps me going is the love of my family – especially my hubby. I know it can be super hard dealing with emotions but make sure to show appreciation to your loved ones! If you ever need a friend to vent to or share your accomplishments, I totally have your back too! 🙂
I hope you find these tips helpful, what about you? Any tips to share for your stroke recovery?